Flexible Low-Temperature RF Plasma Source for Biomedical Applications
Keywords:
engineering in medicine and biology, low-temperature plasmas, optical emission spectroscopy, plasma applications, plasma devicesAbstract
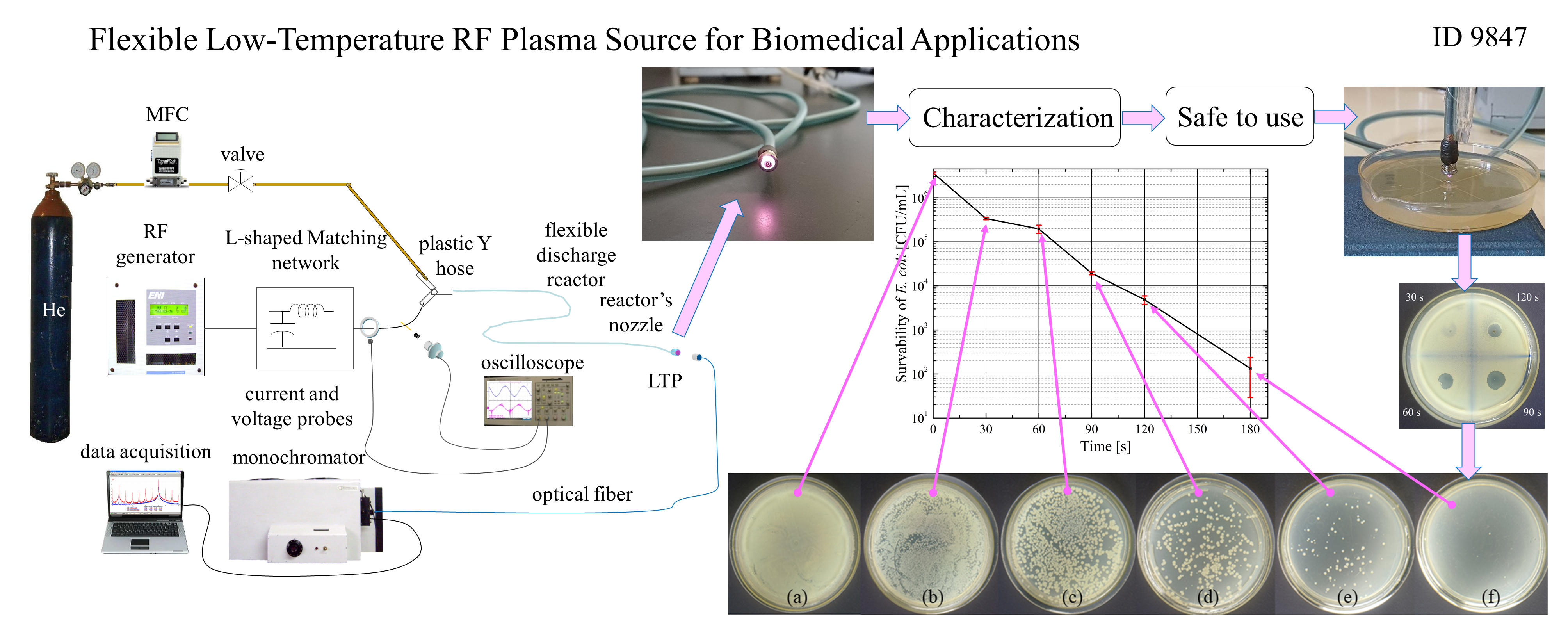
A flexible low-temperature plasma (LTP) source device was developed utilizing a radiofrequency (RF) generator coupled to a coaxial cable through a homemade L-shape matching network and a supple plastic hose that conveys a gas flow and shields the coaxial cable up to the reactor’s nozzle. The impedance matching network provides an electric power transfer of minimum of 94.11% operating under normal conditions. The LTP device arrangement is described, and later characterized via optical emission spectroscopy and electric power consumption. This procedure is essential to determine the adequate application of the generated plasma over heat-sensitive materials, primarily organic matter, to provide adequate information about its physicochemical activity. The produced LTP interacts with surrounding air particles, generating reactive oxygen and nitrogen species (RONS) that exhibit bactericidal and antiseptic properties due to their strong biochemical reactivity. The electromagnetic irradiation, ultraviolet (UV) emission, and thermal surface effect produced under normal working conditions of the LTP source device are safe to apply to heat-sensitive matter. The device’s inactivation property was validated through qualitative deactivation trials of Escherichia coli and Enterococcus faecalis and quantitative deactivation trials of Escherichia coli. The device inactivated 99.996% of E. coli at a concentration of 3.6×106 colony forming units per mL (CFU/mL) in 180 s at 16 W, this result corresponds to a 4.43-log10 reduction in E. coli viability.
Downloads
References
E. Stoffels, et al., “Plasma needle: a non-destructive atmospheric plasma source for fine surface treatment of (bio)materials,” Plasma Sources Sci. Technol., vol. 11, no. 4, pp. 383–388, 2002, doi: 10.1088/0963-0252/11/4/304.
K. Kelly-Wintenberg, et al., “Use of a one atmosphere uniform glow discharge plasma (OAUGDP) to kill a broad spectrum of microorganisms,” J. Vac. Sci. Technol., vol. 17, no. 4, pp. 1539–1544, 1999, doi: 10.1116/1.581849.
S. Lerouge, M. R. Wertheimer and L. Yahia, “Plasma Sterilization: A Review of Parameters, Mechanisms, and Limitations,” Plasmas Polym., vol. 6, pp. 175–188, Sep. 2001, doi: 10.1023/A:1013196629791.
M. Laroussi, “Sterilization of Contaminated Matter with an Atmospheric-Pressure Plasma,” IEEE Trans. Plasma Sci., vol. 24, no. 3, pp. 1188–1191, Jun. 1996. doi: 10.1109/27.533129.
M. Moisan, J. Barbeau, S. Moreau, J. Pelletier, M. Tabrizian and L. H. Yahia, “Low-temperature sterilization using gas plasmas: a review of the experiments and an analysis of the inactivation mechanisms,” Int. J. Pharma., vol. 226, no. 1–2, pp. 1-21, 2001, doi: 10.1016/S0378-5173(01)00752-9.
J. C. Birmingham, “Mechanisms of Bacterial Spore Using Ambient Pressure Nonthermal Discharges,” IEEE Trans. Plasma Sci., vol. 32, no. 4, pp. 1526–1531, Aug. 2004, doi: 10.1109/TPS.2004.832609.
T. Nosenko, T. Shimizu and G. E. Morfill, “Designing plasmas for chronic wound disinfection,” New J. Phys, vol. 11, Nov. 2009, Art. no. 115013, doi: 10.1088/1367-2630/11/11/115013.
J. Goree, B. Liu, D. Drake and E. Stoffels, “Killing of S. mutans Bacteria Using a Plasma Needle,” IEEE Trans. Plasma Sci., vol. 34, no. 4, pp. 1317–1324, Aug. 2006. doi: 10.1109/TPS.2006.878431
T. C. Montie, K. Kelly-Wintenberg and J. R. Roth, “An Overview of Research Using the One Atmosphere Uniform Glow Discharge Plasma (OAUGDP) for Sterilization of Surfaces and Materials,” IEEE Trans. Plasma Sci., vol. 28, no. 1, pp. 41–50, Feb. 2000, doi: 10.1109/27.842860
E. Stoffels, I. E. Kieft and R. E. J. Sladek, “Superficial treatment of mammalian cells using plasma needle,” J. Phys. D: Appl. Phys., vol. 36, pp. 2908–2913, 2003. [Online]. Available: stacks.iop.org/JPhysD/36/2908.
D. Dobrynin, G. Fridman, G. Friedman and A. Fridman, “Physical and biological mechanisms of direct plasma interaction with living tissue,” New J. Phys, vol. 11, Nov. 2009, Art. no. 115020, doi: 10.1088/1367-2630/11/11/115020.
S. Coulombe, V. Léveillé, S. Yonson and R. L. Leask, “Miniature atmospheric pressure glow discharge torch (APGD-t) for local biomedical applications,” Pure Appl. Chem., vol. 78, no. 6, pp. 1147–1156, 2006, doi: 10.1351/pac200678061147.
X. M. Shi, et al., “Low-temperature Plasma Promotes Fibroblast Proliferation in Wound Healing by ROS-activated NF-κB Signaling Pathway,” Curr Med Sci., vol. 38, no. 1, pp. 107–114, Feb. 2018, doi: 10.1007/s11596-018-1853-x.
E. García-Alcántara, et al., “Accelerated mice skin acute wound healing in vivo by combined treatment of argon and helium plasma needle,” Arch. Med. Res., vol. 44, pp. 169–177, 2013, doi: 10.1016/j.arcmed.2013.02.001.
M. Chatraie, G. Torkaman, M. Khani, H. Salehi and B. Shokri, “In vivo study of non-invasive effects of non-thermal plasma in pressure ulcer treatment,” Sci. Reports, vol. 8, 2018, Art. no. 5621, doi: 10.1038/s41598-018-24049-z.
S. K. Dubey, et al., “Cold atmospheric plasma therapy in wound healing,” Process Biochem., vol. 112, pp. 112–123, 2022, doi: 10.1016/j.procbio.2021.11.017.
G. Fridman et al., “Floating Electrode Dielectric Barrier Discharge Plasma in Air Promoting Apoptotic Behavior in Melanoma Skin Cancer Cell Lines,” Plasma Chem. Plasma Proc., vol. 27, pp. 163–176, 2007, doi: 10.1007/s11090-007-9048-4.
X. Yan, et al., “On the Mechanism of Plasma Inducing Cell Apoptosis,” IEEE Trans. Plasma Sci., vol. 38, no. 9, pp. 2451–2457, Sep. 2010, doi: 10.1109/TPS.2010.2056393.
H. J. Lee, C. H. Shon, Y. S. Kim, S. Kim, G. C. Kim and M. G. Kong, “Degradation of adhesion molecules of G361 melanoma cells by a non-thermal atmospheric pressure microplasma,” New J. Phys., vol. 11, 2009, Art. no. 115026, doi: 10.1088/1367-2630/11/11/115026.
J. H. Serment Guerrero, K. Girón-Romero, R. López-Callejas and R. Peña-Eguiluz, “In vitro assessment of murine melanoma cells sensitivity to non-thermal atmospheric plasma,” J. Appl. Res. Technol., vol. 17, pp. 180–185, 2019. [Online]. Available: https://jart.icat.unam.mx/index.php/jart/article/
view/810/743
I. Adamovich, et al., “The 2022 Plasma Roadmap: low temperature plasma science and technology,” J. Phys. D: Appl. Phys., vol. 55, pp. 22–25, 2022, Art. no. 373001, doi: 10.1088/1361-6463/ac5e1c.
M. Betancourt-Ángeles et al., “Treatment in the healing of burns with a cold plasma source,” Int. J. Burns Trauma, vol. 7, pp. 142–146, 2017. [Online]. Available: https://pmc.ncbi.nlm.nih.gov/articles/PMC5768930/
C. Duchesne, S. Banzet, J.-J. Lataillade, A. Rousseau and N. Frescaline, “Cold atmospheric plasma modulates endothelial nitric oxide synthase signalling and enhances burn wound neovascularization,” J. Pathology, vol. 249, no. 3, pp. 368–380, nov. 2019, doi: 10.1002/path.5323.
R. Peña-Eguiluz, R. López-Callejas, B. González-Mendoza, A. Mercado-Cabrera, B. G. Rodríguez-Mendez and R. Valencia-Alvarado, “Acute Neck Radiodermatitis Treated by Nonthermal Plasma Therapy: Case Report,” IEEE Trans. Rad. Plasma Med. Sci., vol. 6, no. 4, pp. 503–506, Apr. 2022, doi: 10.1109/TRPMS.2021.3070784.
A. Chuangsuwanich, T. Assadamongkol and D. Boonyawan, “The Healing Effect of Low-Temperature Atmospheric-Pressure Plasma in Pressure Ulcer: A Randomized Controlled Trial,” Int. J. Lower Extremity Wounds, vol. 15, no. 4, pp. 313–319, aug. 2016, doi:10.1177/1534734616665046.
B. González-Mendoza, et al., “Healing of wounds in lower extremities employing a non-thermal plasma,” Clinical Plasma Med., vol. 16, 2019, Art. no. e100094, doi: 10.1016/j.cpme.2020.100094.
R. López-Callejas et al., “Alternative method for healing the diabetic foot by means of a plasma needle,” Clinical Plasma Med., vol. 9, pp. 19–23, 2018, doi: 10.1016/j.cpme.2018.01.001.
R. He, et al., “The efficacy and safety of cold atmospheric plasma as a novel therapy for diabetic wound in vitro and in vivo,” Int. Wound J., vol. 17, no. 3, pp. 851–863, Jun. 2020; doi: 10.1111/iwj.13341
R. Peña-Eguiluz, et al., “Non-thermal plasma wound healing after removal of a neck tumor in a patient with HIV: A case report,” Otolaryngology Case Reports, vol. 22, Jan. 2022, Art. no. 100391, doi: 10.1016/j.xocr.2021.100391.
N. G. Ibáñez-Mancera, et al., “Wound Healing After Biopsy in the Mobile Oral Mucosa Using a Nonthermal Atmospheric Pressure Plasma,” IEEE Trans. Rad. Plasma Med. Sci., vol. 6, no. 8, pp. 928–935, Nov. 2022, doi: 10.1109/TRPMS.2022.3161188
N. G. Ibáñez-Mancera, et al., “Healing of Recurrent Aphthous Stomatitis by Non-Thermal Plasma: Pilot Study,” Biomedicines, vol. 11, 2023, Art. no. 167, doi: 10.3390/biomedicines11010167.
M. Vandamme, et al., “ROS implication in a new antitumor strategy based on non-thermal plasma,” Int. J. Cancer, vol. 130, no. 9, pp. 2185–2194, May 2012, doi: 10.1002/ijc.26252.
S. Kang, et al., “Nonthermal plasma induces head and neck cancer cell death: the potential involvement of mitogen-activated protein kinase-dependent mitochondrial reactive oxygen species,” Cell Death Dis., vol. 5, 2014, Art. no. e1056, doi:10.1038/cddis.2014.33.
C. Song, P. Attri, S. K. Ku, I. Han, A. Bogaerts and E H. Choi, “Cocktail of reactive species generated by cold atmospheric plasma: oral administration induces non-small cell lung cancer cell death,” J. Phys. D: Appl. Phys., vol. 54, no. 18, 2021, Art. no. 185202, doi: 10.1088/1361-6463/abdff2.
H. Tanaka, S. Bekeschus, D. Yan, M. Hori, M. Keidar and M. Laroussi, “Plasma-Treated Solutions (PTS) in Cancer Therapy”, Cancers, vol. 13, no. 7, Apr. 2021, Art. no. 1737, doi: 10.3390/cancers13071737.
G. Neretti, et al., “Characterization of a plasma source for biomedical applications by electrical, optical, and chemical measurements,” Plasma Proc. Polym., vol. 15, no. 11, Nov. 2018, Art. no. 1800105, doi: 10.1002/ppap.201800105.
T. von Woedtke, M Laroussi and M Gherardi, “Foundations of plasmas for medical applications,” Plasma Sources Sci. Technol., vol. 31, no. 5, 2022, Art. no. 054002, doi: 10.1088/1361-6595/ac604f.
K.-D. Weltmann and T. von Woedtke, “Basic requirements for plasmas sources in medicine,” Eur. Phys. J.: Appl. Phys., vol. 55, Jul. 2011, Art. no. 13807, doi: 10.1051/epjap/2011100452.
R. Peña-Eguiluz, et al., “Development and Characterization of a Non-Thermal Plasma Source for Therapeutic Treatments”, IEEE Trans. Biomed. Eng., vol. 68, no. 5, pp. 1467–1476, May 2021, doi: 10.1109/TBME.2020.3041195.
T. Liu, et al., “Design of a Flexible Microwave-Induced Room-Temperature Atmospheric-Pressure Microwave Source,” IEEE Trans. Plasma Sci., vol. 52, no. 3, pp. 652–656, Mar. 2024, doi: 10.1109/TPS.2024.3376526.
C. Corbella and S. Portal, “Flexible plasma multi-jet source operated in radial discharge configuration,” Rev. Sci. Instrum., vol. 92, no. 12, Dec. 2021, Art. no. 123502, doi: 10.1063/5.0068219.
O. Bastin, et al., “Optical and Electrical Characteristics of an Endoscopic DBD Plasma Jet,” Plasma Med., vol. 10, no. 2, pp 71–90, 2020, doi: 10.1615/PlasmaMed.2020034526.
F. do Nascimento, et al., “A Low Cost, Flexible Atmospheric Pressure Plasma Jet Device with Good Antimicrobial Efficiency,” IEEE Trans. Rad. Plasma Med. Sci., vol. 8, no. 3, pp. 307–322, Mar. 2024, doi: 10.1109/TRPMS.2023.3342709.
International Commission on Non-Ionizing Radiation Protection, “ICNIRP statement on diagnostic devices using non-ionizing radiation: Existing regulations and potential health risks,” Health Phys., vol. 112, no. 3, pp. 305–321, Jan. 2017, doi: 10.1097/HP.0000000000000654.
R. W. B. Pearse and A. G. Gaydon, The identification of molecular spectra, London, England: Chapman & Hall LTD., 1941, pp. 1–276. [Online]. Available: https://archive.org/details/in.ernet.dli.2015.212925.
A. G. Gaydon, “The band spectrum of NO: The gamma and epsilon systems,” Proc. Phys. Society, vol. 56, no. 2, pp. 95–-103, 1944, doi: 10.1088/0959-5309/56/2/305.
S. Reuter, T. von Woedtke and K.-D. Weltmann, “The kINPen–a review on physics and chemistry of the atmospheric pressure plasma jet and its applications,” J. Phys. D: Appl. Phys., vol. 51, no. 23, 2018, Art. no. 233001, doi: 10.1088/1361-6463/aab3ad.
V. V Kovačević, B. P. Dojčinović, M. Jović, G. M. Roglić, B. M. Obradović and M. M. Kuraica, “Measurement of reactive species generated by dielectric barrier discharge in direct contact with water in different atmospheres,” J. Phys. D: Appl. Phys., vol. 50, 2017, Art. no. 155205, doi: 10.1088/1361-6463/aa5fde.
S. Wang, D. Yang, F. Liu, W. Wang and Z. Fang, “Spectroscopic study of bipolar nanosecond pulse gas-liquid discharge in atmospheric argon,” Plasma Sci. Technol., vol. 20, no. 7, 2018, Art. no. 075404, doi: 10.1088/2058-6272/aabac8.
I. A. Kossyi, A. Y. Kostinsky, A. A. Matveyev and V. P. Silakov, “Kinetic scheme of the non-equilibrium discharge in nitrogen-oxygen mixtures,” Plasma Sources Sci. Technol., vol. 1, no. 3, pp. 207–220, 1992, doi: 10.1088/0963-0252/1/3/011.
N. G. Ibáñez-Mancera, et al., “Cold Atmospheric Plasma Benefits after a Biopsy on the Gingiva and Palate: A Case Series," Plasma Med, vol. 12, no. 4, pp. 1–9, Dec. 2022, doi: 10.1615/PlasmaMed.2022045686
K. P. Ha, R. S. Clarke, G. Kim, J. L. Brittan, J. E. Rowley, et al., “Staphylococcal DNA repair is required for infection”, mBio, vol. 11, no. 6, 2020, doi: 10.1128/mbio.02288-20.
L. Pinard, and C. Batiot-Dupeyrat, “Non-thermal plasma for catalyst regeneration: A review,” Catal. Today, vol. 426, Jan. 2024, Art. no. 114372, doi: 10.1016/j.cattod.2023.114372.
Y. Xu, and A. Bassi, “Non-thermal plasma decontamination of microbes: a state of the art,” Biotechnol. Prog., vol. 41, no. 2, Mar.-Apr. 2025, Art. no. e3511, doi: 10.1002/btpr.3511.
S. G. Scaltriti, A. Cristofolini, and G. Neretti, “Design and Characterization of an Atmospheric Pressure Dielectric Barrier Discharge Reactor for Potential Air Disinfection Applications,” IEEE Access, vol. 13, Mar. 2025, Art. no. e45037, doi: 10.1109/ACCESS.2025.3548933.
A. Helmke, I. Curril, J. Mrotzek, J. Schulz, and W. Viöl. “Non-thermal plasma for decontamination of bacteria trapped in particulate matter filters: plasma source characteristics and antibacterial potential,” J. Phys. D: Appl. Phys., vol. 57, no. 26, Apr. 2024, Art no. 265202, doi: 10.1088/1361-6463/ad35d3.
A. H. Marx, H. Oltmanns, J. Meißner, J. Verspohl, T. Fuchsluger, and C. Busse. “Argon cold atmospheric plasma eradicates pathogens in vitro that are commonly associated with canine bacterial keratitis,” Front. Vet. Sci., vol, 10, 2023, Art. no. 1320145, doi: 10.3389/fvets.2023.1320145.
J. Stoof, et al., “Non-thermal plasma as promising anti-cancer therapy against bladder cancer by inducing DNA damage and cell cycle arrest,” Sci. Rep., vol. 1, Jan. 2025, Art. no. 2334, doi: 10.1038/s41598-025-85568-0.
R. Shoorgashti, R. Nikmaram, Y. Azimi, A. Rouientan, H. Ebrahimi, and S. Lesan, “Effectiveness of cold plasma application in oral wound healing process: A scoping review,” Oral Dis., vol. 30, no. 8, pp. 5062–5081, Nov. 2024, doi: 10.1111/odi.15119.
E. Biscop, et al., “Dose-dependent induction of epithelial-mesenchymal transition in 3D melanoma models by non-thermal plasma treatment,” Mol. Oncol., early access, doi: 10.1002/1878-0261.70055.
T. Sharfuddin, D. Jacho, D. Mitchey, E. Yildirim-Ayan, and H. Ayan, “A Study on the Effect of Non-thermal Plasma on Macrophage Phenotype Modulation,” Plasma Chem. Plasma Proc., vol. 44, pp. 455–470, Jan. 2024, doi: 10.1007/s11090-023-10414-y.
T. Dufour, “From Basics to Frontiers: A Comprehensive Review of Plasma-Modified and Plasma-Synthesized Polymer Films,” Polymers, vol. 15, no. 17, 2023, Art. no. 3607, doi: 10.3390/polym15173607.
M. A. Ansari, et al., “Characterization of Plasma Discharge in a Multi Dipole Line Cusp Magnetic Field Created by an RF Source Coupled by a Spiral Antenna,” IEEE Trans. Plasma Sci., vol. 51, no. 3, pp. 625–631, Mar. 2023, doi: 10.1109/TPS.2023.3251384.
J. E. Thomas and K. Stapelmann, “Plasma Control: A Review of Developments and Applications of Plasma Medicine Control Mechanisms,” Plasma, vol. 7, no. 2, pp. 386–426, May 2024, doi: 10.3390/plasma7020022.
A. Zerehpoush, Z. R. Mobaraki, H. Afarideh and H. Rahimpour, “An Automatic Impedance Matching Network Based on Neural Network Technique for Inductive RF Plasma Source,” IEEE Trans. Instrum. Meas., vol. 74, Mar. 2025, Art. no. 2513009, doi: 10.1109/TIM.2025.3544285.
J. Apelqvist, et al., “Cold plasma: an emerging technology for clinical use in wound healing,” J. Wound Manage., vol. 25, no. 3, pp. S1–S84, 2024; doi: 10.35279/jowm2024.25.03.sup01.
H. R. Lee, et al., “Liquid plasma as a treatment for cutaneous wound healing through regulation of redox metabolism,” Cell Death Dis., vol 14, Feb. 2023, Art. no. 119, doi: 10.1038/s41419-023-05610-9.