Cardiac Ischemia Detection Using Parameters Extracted from the Intrinsic Mode Functions
Keywords:
Electrocardiogram, Empirical Mode Decomposition, Hilbert Transform, Hjorth ActivityAbstract
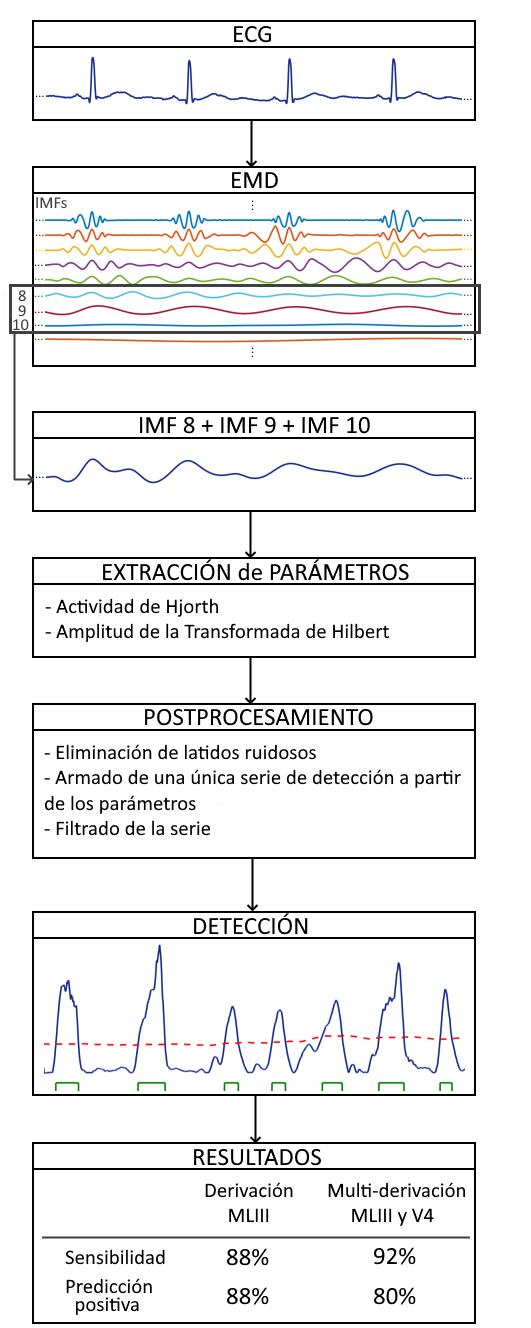
Cardiac ischemia is the main cause of death in the world, thus the importance of prevention and early detection of these events. Traditionally, ischemia is detected by analyzing the alteration of the ST level in the electrocardiogram (ECG). In this study, we propose two new parameters extracted from the ECG to improve the cardiac ischemia detection. For this, the signal was decomposed using the Empirical Mode Decomposition, and the Intrinsic Mode Functions related to the frequency band of the ST level were selected. From these modes, two parameters were obtained: the Hjorth Activity and the frequency amplitude, using the Hilbert Transform. With these parameters, two analyses were done. First, the parameters obtained during normal periods were compared with those obtained during ischemic events. Second, a temporal series was obtained with both parameters, where the detection was done using an adaptative threshold. Results were obtained using all the patients with MLIII lead of the European ST-T Database. Parameters differed significantly across ischemic and non ischemic episodes, obtaining a sensitivity and positive predictive value of 88%, after removing noisy records. Also, a multi-lead detection was performed in patients with MLIII and V4 leads. The sensitivity and positive predictive value obtained were 92% and 80%, respectively.
Downloads
References
W. H. Organization, “Global Health Estimates 2020: Deaths by Cause, Age, Sex, by Country and by Region, 2000-2019,” tech. rep., Geneva, 2020.
L. Sörnmo and P. Laguna, “The Electrocardiogram - A Brief Background,” in Bioelectrical Signal Processing in Cardiac and Neurological Applications, ch. 6, p. 411, Academic Press, 2005.
J. Cinca, F. J. Noriega, E. Jorge, J. Alvarez-Garcia, G. Amoros, and D. Arzamendi, “St-segment deviation behavior during acute myocardial ischemia in opposite ventricular regions: Observations in the intact and perfused heart,” Heart Rhythm, vol. 11, no. 11, pp. 2084–2091, 2014.
G. D. Clifford, F. Azuaje, and P. E. McSharry, Advanced Methods and Tools for ECG Data Analysis. Artech House, 2006.
A. Gallina, S. Chierchia, G. Smith, M. Croom, M. Morgan, C. Marchesi, and A. Maseri, “Computer system for analysis of ST segment changes on 24 hour Holter monitor tapes: Comparison with other available systems,” Journal of the American College of Cardiology, vol. 4, no. 2, pp. 245–252, 1984.
A. Taddei, G. Costantino, R. Silipo, M. Emdin, and C. Marchesi, “A system for the detection of ischemic episodes in ambulatory ECG,” Computers in Cardiology, pp. 705–708, 1995.
J. García, L. Sörnmo, S. Olmos, and P. Laguna, “Automatic detection of ST-T complex changes on the ECG using filtered RMS difference series: Application to ambulatory ischemia monitoring,” IEEE Transactions on Biomedical Engineering, vol. 47, no. 9, pp. 1195–1201, 2000.
G. Sun, C. W. Thomas, J. Liebman, Y. Rudy, Y. Reich, O. Stilli, and E. Macchi, “Classification of normal and ischemia from BSPM by neural network approach,” in Proceedings of the Annual International Conference of the IEEE Engineering in Medicine and Biology Society, 1988.
F. Jager, G. B. Moody, and R. G. Mark, “Detection of transient ST segment episodes during ambulatory ECG monitoring.,” Computers and biomedical research, an international journal, vol. 31, no. 5, pp. 305–22, 1998.
A. Smrdel and F. Jager, “Automated detection of transient ST-segment episodes in 24 h electrocardiograms.,” Medical & biological engineering & computing, vol. 42, no. 3, pp. 303–311, 2004.
P. Ranjith, P. C. Baby, and P. Joseph, “ECG analysis using wavelet transform: application to myocardial ischemia detection Détection des événements ischémiques myocardiques à partir de la transformée en ondelettes du signal ECG,” Engineering, vol. 24, pp. 44–47, 2003.
D. Lemire, C. Pharand, J. C. Rajaonah, B. Dubé, and A. Robert Leblanc, “Wavelet time entropy, T wave morphology and myocardial ischemia,” IEEE Transactions on Biomedical Engineering, vol. 47, no. 7, pp. 967–970, 2000.
T. Stamkopoulos, K. Diamantaras, N. Maglaveras, and M. Strintzis, “ECG analysis using nonlinear PCA neural networks for ischemia detection,” IEEE Transactions on Signal Processing, vol. 46, no. 11, pp. 3030–3044, 1998.
F. Jager, R. Mark, G. Moody, and S. Divjak, “Analysis of Transient ST Segment Changes During Ambulatory Monitoring,” Computers in Cardiology 1991, Proceedings., pp. 453 – 456, 1991.
S. Papadimitriou, S. Mavroudi, L. Vladutu, and A. Bezerianos, “Ischemia detection with a self-organizing map supplemented by supervised learning,” IEEE Transactions on Neural Networks, vol. 12, no. 3, pp. 503–515, 2001.
A. K. Manocha and M. Singh, “An Overview of Ischemia Detection Techniques,” International Journal of Scientific & Engineering Research, Volume 2, Issue 11, vol. 2, no. 11, pp. 1–5, 2011.
S. Ansari, N. Farzaneh, M. Duda, K. Horan, H. B. Andersson, Z. D. Goldberger, B. K. Nallamothu, and K. Najarian, “A review of automated methods for detection of myocardial ischemia and infarction using electrocardiogram and electronic health records,” IEEE Reviews in Biomedical Engineering, vol. 10, pp. 264–298, 2017.
A. Taddei, G. Distante, M. Emdin, P. Pisani, G. Moody, C. Zeelenberg, and C. Marchesi, “The European ST-T database standard for evaluating systems for the analysis of ST-T changes in ambulatory electrocardiography,” European Heart Journal, vol. 13, pp. 1164–1172, 1992.
A. Goldberger, L. Amaral, L. Glass, J. Hausdorff, P. Ivanov, R. Mark, J. Mietus, G. Moody, C. Penk, and H. Stanley, “PhysioBank, PhysioToolkit, and PhysioNet: components of a new research resource for complex physiologic signals.,” Circulation, vol. 23, pp. e215–e220, 2000.
N. E. Huang and S. S. P. Shen, Hilbert-Huang Transform and Its Applications. Interdisciplinary Mathematical Sciences, 2005.
C. Fernández Biscay, P. D. Arini, A. I. Rincón Soler, and M. P. Bonomini, “Classification of ischemic and non-ischemic cardiac events in Holter recordings based on the continuous wavelet transform,” Medical and Biological Engineering and Computing, vol. 58, no. 5, pp. 1069–1078, 2020.
B. Hjorth, “EEG Analysis Based on Time Domain Properties,” Electroencephalography and Clinical Neurophysiology, vol. 29, pp. 306–310, 1970.
G. B. Moody and R. G. Mark, “Development and evaluation of a 2-lead ECG analysis program,” Computers in Cardiology, pp. 39–44, 1982.
C. R. Meyer and H. N. Keiser, “Electrocardiogram baseline noise estimation and removal using cubic splines and state-space computation techniques,” Computers and Biomedical Research, vol. 10, no. 5, pp. 459–470, 1977.
A. J. Demski and M. L. Soria, “ecg-kit a Matlab Toolbox for Cardiovascular Signal Processing,” Journal of Open Research Software, vol. 4, pp. 2–5, 2016.
A. Kabir and C. Shahnaz, “Denoising of ECG signals based on noise reduction algorithms in EMD and wavelet domains,” Biomedical Signal Processing and Control, vol. 7, no. 5, pp. 481–489, 2012.
A. Kumar and M. Singh, “Statistical analysis of ST segments in ECG signals for detection of ischaemic episodes,” Transactions of the Institute of Measurement and Control, vol. 40, no. 3, pp. 819–830, 2018.
M. Rakshit and S. Das, “An efficient ECG denoising methodology using empirical mode decomposition and adaptive switching mean filter,” Biomedical Signal Processing and Control, vol. 40, pp. 140–148, 2018.
P. Sharma and K. C. Ray, “Efficient methodology for electrocardiogram beat classification,” IET Signal Processing, vol. 10, no. 7, pp. 1–8, 2016.
M. Suchetha and N. Kumaravel, “Classification of arrhythmia in electrocardiogram using EMD based features and support vector machine with margin sampling,” International Journal of Computational Intelligence and Applications, vol. 12, no. 3, pp. 1350015–13, 2013.
R. M. Mehmood and H. J. Lee, “EEG based Emotion Recognition from Human Brain using Hjorth Parameters and SVM,” International Journal of Bio-Science and Bio-Technology, vol. 7, no. 3, pp. 23–32, 2015.
M. Tanveer, “Classification of seizure and seizure-free EEG signals using Hjorth parameters,” 2018 IEEE Symposium Series on Computational Intelligence (SSCI), 2018.
M. S. Safi and S. M. M. Safi, “Early detection of Alzheimer’s disease from EEG signals using Hjorth parameters,” Biomedical Signal Processing and Control, vol. 65, 2021.
S. Hadiyoso, S. Aulia, and A. Rizal, “One-Lead Electrocardiogram for Biometric Authentication using Time Series Analysis and Support Vector Machine,” International Journal of Advanced Computer Science and Applications, vol. 10, no. 2, pp. 276–283, 2019.
J. P. R. Leite and R. L. Moreno, “Heartbeat classification with low computational cost using Hjorth parameters,” IET Signal Processing, vol. 12, no. 4, pp. 431–438, 2018.
S. Hadiyoso and A. Rizal, “Electrocardiogram Signal Classification Using Higher-Order Complexity of Hjorth Descriptor,” Advanced Science Letters, vol. 23, no. 5, pp. 3972–3974, 2017.
Sivaraman Jayaraman, V. Sangareddi, R. Periyasamy, J. Joseph, and R. M. Shanmugam, “Modified limb lead ECG system effects on electrocardiographic wave amplitudes and frontal plane axis in sinus rhythm subjects,” Anatol J Cardiol., vol. 17, no. 1, pp. 46–54, 2017.
J. Vila, J. Presedo, M. Delgado, S. Barro, R. Ruiz, and F. Palacios, “SUTIL: Intelligent ischemia monitoring system,” International Journal of Medical Informatics, vol. 47, pp. 193–214, 1997.
N. Maglaveras, T. Stamkopoulos, C. Pappas, and M. G. Strintzis, “An adaptive backpropagation neural network for real-time ischemia episodes detection: Development and performance analysis using the European ST-T database,” IEEE Transactions on Biomedical Engineering, vol. 45, no. 7, pp. 805–813, 1998.
A. Bezerianos, L. Vladutu, and S. Papadimitriou, “Hierarchical state space partitioning with a network self-organising map for the recognition of ST-T segment changes,” Medical & Biological Engineering & Computing, vol. 38, no. 4, pp. 406–415, 2000.
M. Wasimuddin, K. Elleithy, A. Abuzneid, M. Faezipour, and O. Abuzaghleh, “ECG Signal Analysis Using 2-D Image Classification with Convolutional Neural Network,” 2019 International Conference on Computational Science and Computational Intelligence (CSCI), 2019.
A. F. Hussein, S. J. Hashim, F. Z. Rokhani, and W. A. Wan Adnan, “An Automated High-Accuracy Detection Scheme for Myocardial Ischemia Based on Multi-Lead Long-Interval ECG and Choi-Williams Time-Frequency Analysis Incorporating a Multi-Class SVM Classifier,” Sensors, vol. 21, no. 7, 2021.
I. Ogrezeanu, D. Stoian, A. Turcea, and L. M. Itu, “Deep learning based myocardial ischemia detection in ECG signals,” 2020 24th International Conference on System Theory, Control and Computing (ICSTCC), 2020.